
Photo by Mary L. Williams
Scaly Skin and Ichthyosis
Probably everybody at some point notices some flakes – some scales – on their skin. Maybe some dry patches on the lower legs? Or the peeling that happens after a sunburn. But most of the time our skin – if it is healthy – doesn’t produce visible scales or flakes. Instead we shed our skin invisibly, single invisible cell by single invisible cell.
But some people are born with a condition in which visible scales accumulate on most or all of their skin surface. This condition, called ‘ichthyosis‘, we now recognize is not just one thing, but instead represents a whole family of inherited conditions that have this feature in common.
Although each member of the ichthyosis family may be quite uncommon to rare, as we learn about their underlying genetic causes, these conditions are teaching us a lot about how the skin works.
To Scale Or Not
Scales are what we see when the outermost cells of our skin are no longer being shed invisibly, one by one, but instead remain clumped together and loosely attached. The shedding process, normally orderly and invisible, has now become disorderly and highly visible.
‘Desquamation’ is the name for the mechanism whereby dead skin cells or ‘squames’ are discarded from the outermost layer of skin, the stratum corneum. Normally, desquamation occurs single cell by single cell, and is imperceptible to the naked eye. This process is aided by the friction arising from our daily activities, and is further assisted by bathing.
But when shedding is abnormal (or ‘pathological’) for some reason, the squames fail to detach as individuals. Instead they remain stuck together in large and now-visible aggregates.
Common examples of pathological desquamation that many of us experience at some time in our lives include the clumps of scale in dandruff, or the sheets of dead skin that peel away several days following a sunburn. Abnormal desquamation is also another sign of the common condition, ‘dry’ skin ( or ‘xerosis’). In other common skin conditions, like eczema (or atopic dermatitis) or psoriasis, visible scales are often present.
Nothing To Do With Fish
In the family of inherited disorders called ichthyosis, scaling is often the most prominent feature and may affect most or all of the skin.
The term ‘ichthyosis’ comes from the Greek root for fish, ‘ichthys.’ These are medical conditions and, of course, they have nothing to do with fish and fish skin! This fanciful name was acquired hundreds of years ago, when many skin disorders were called by what they seemed to mimic in nature. More accurate and less pejorative terms, like ‘disorders of keratinization’ or ‘disorders of cornification’ (our preference), are a mouthful, and, thus for better or worse, the term ‘ichthyosis’ remains firmly entrenched in the medical lexicon.

Most members of this large family are quite rare, although a couple of them are more common. Indeed, one common form is named ‘ichthyosis vulgaris’, not because the condition is ‘vulgar,’ in our sense of the word, but because ‘vulgaris’ means ‘common’ in Latin. Other forms of ichthyosis are so uncommon, that were it not for the internet, through social media and FIRST (the Foundation for Ichthyosis and Related Skin Types), an individual with one of these rarer forms of ichthyosis might go through his or her entire life without ever encountering another, similarly affected person.
While it can be a challenge for someone with ichthyosis to deal with his or her skin disorder, these genetic diseases can be a real boon to scientists who wish to understand how the skin works.
Scientists typically design experiments to study complex systems – like human diseases – by altering a single component in a model system, and then observing what happens. The result of their experiment then allows the scientist to infer how that one piece of the puzzle operates within the larger system.
Simple (or ‘Mendelian’) genetic conditions, in which only a single gene is altered or ‘mutated’, can provide scientists with built-in experiments, designed by nature. Because the ichthyoses are such single gene traits, they can offer skin scientists with clues about how the process of skin shedding occurs normally, by allowing them to discover what happens when nature tinkers with one part of this process.
How To Shed Skin
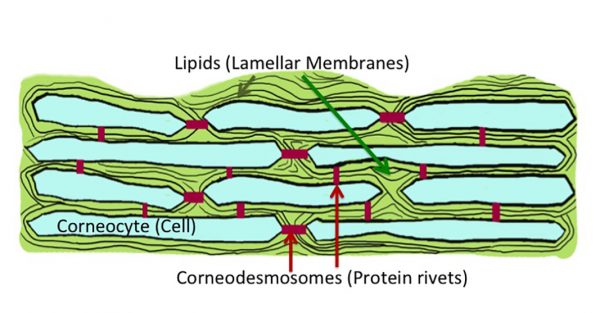
The ichthyoses have indeed taught us a lot about the process of desquamation. One of the key players in this process are a family of proteins that form structures, called ‘corneodesmosomes’, that weld the stratum corneum cells (or ‘corneocytes’) together. These corneodesmosomes allow the corneocytes to form a multi-tiered structure of interlocked cells – the stratum corneum. They hold the cells tightly attached one to another (so they don’t shed).
To enable the squames to detach, something has to break up the corneodesmosomes that bind them together. These power-drills are a family of enzymes called ‘proteases,’ which digest proteins into small pieces.
Normally, these rivets between adjacent corneocytes are gradually eaten away by the proteases, as new cells push them upward and outward towards the skin surface. By the time the cells reach the surface, their corneodesmosome connectors have been reduced to a few, weak remnants. Now with the mild friction of daily activities, the loosely held squames can detach from one another and to be swept away.
Missing In Action
In some of the ichthyoses, there is a problem in the delivery of proteases to the right place. They don’t get to the region outside the cells where their protein ‘diet’ – the corneodesmosomes – reside. Although in this case, the epidermal cells make the necessary proteases, but there is a delivery problem. The proteases remain trapped inside the cells, and unable to reach the region between the cells where the corneodesmosomes reside.
Consider this problem as analogous to a strike by truck drivers at a furniture factory. Sofas and chairs begin to clog the warehouses, because these products cannot be shipped out to their buyers.
This type of problem is encountered in the form of ichthyosis called ‘harlequin ichthyosis‘. Here there is a protein missing (called ABCA12) that is needed to fill the lamellar bodies (the trucks, in our example) with their critical ingredients, which include both the skin’s water proofing fats (‘lipids’) but also its digestive enzymes, its proteases.
In other cases, the proteases are where they need to be – that is, their delivery is unimpeded – but they are being held captive in an inactive or inhibited state, and are unable to do their digestive work. In this case, it is as if the workers on the other end who receive the products are on strike, and refuse to unload them from the delivery vans.
This is the mechanism underlying the scaling in X-linked ichthyosis. Here the missing enzyme, ‘steroid sulfatase’, leads to an accumulation of its ‘food’ cholesterol sulfate, in stratum corneum. Cholesterol sulfate prevents the key proteases from digesting the corneodesmosomes – and the accumulation of visible scales is the result.
Too Soon
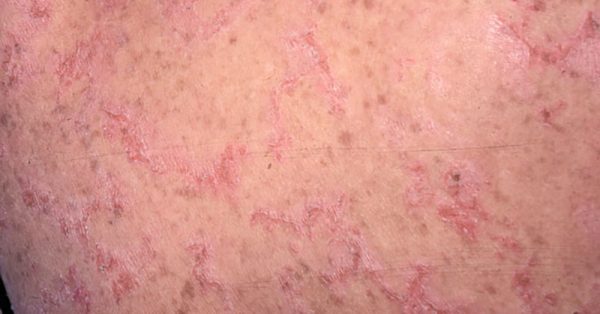
In still other ichthyoses, like Netherton syndrome, the problem is that the proteases become active too soon. This happens when other proteins – ‘inhibitors’ – that are charged with holding the proteases in check until it is time for the squames to be shed – are missing. The activity of these proteases need to be managed, so that they are turned on at the right time. Turned on too soon – because a key inhibitor is missing – the corneodesmosome rivets are digested too quickly and the stratum corneum is shed too soon.
Another form of ichthyosis, peeling skin disease, can be due to a defect in one of the proteins of the corneodesmosome themselves, resulting in weakened bridges. In both of these instances, the skin is scaly because the stratum corneum is being shed too soon – abruptly, and in large sheets of cells – rather than too late, as in the previous examples.
While in most types of ichthyosis, scaling is part of having a stratum corneum that is thicker than it should be, in these two examples, Netherton syndrome and peeling skin disease, the stratum cornuem is thinner than normal.
Too Many
In a number of the ichthyoses, the problem is one of too much too soon. Too many cells are being produced and they speed too rapidly towards the stratum corneum, arriving there in an unfinished, immature state.
In these cases, the epidermis is ‘hyperproliferative’ – it is multiplying too rapidly. The result is a flood of new cells into the stratum corneum, cells which often have not had time to mature into fully differentiated, cornified cells.
This is a bit like a freeway at rush hour, perhaps in an impoverished region. Not only is the highway flooded with cars, but the cars are old and frequently experience mechanical problems, further backing up traffic. These hastily formed, immature cells have not totally completed their synthesis and secretion of the proteases needed to mediate desquamation. This situation is not limited to the inherited ichthyoses. The scaling that is seen in the inflammatory disease, psoriasis, also reflects this type of dysfunction.
As Simple As pH
One way the proteases involved in desquamation are held in check is by altering the hydrogen ion concentration (or the pH) around them. A high concentration of hydrogen ions results in a low or acidic pH. Normally, the interior of the body has close to a neutral pH. But by the time a skin cell reaches the outer skin surface, the pH has become quite acidic, in the range of pH4.5 to 5.0.
In several skin diseases that affect the stratum corneum, including the ichthyoses, this normal pH balance is disturbed, and the surface becomes less acidic (or more ‘basic’). Most enzymes – including these important proteases – have a limited range of preferences for pH. Their ability to digest proteins very much depends on the pH of the environment around them. While some of the proteases, prefer an acidic pH, while others are more active at a more neutral pH. Hence, when the pH of the stratum corneum is abnormal, desquamation inevitably is abnormal as well.
The scaling in atopic dermatitis is due in part to an increased surface pH, activating proteases that prefer a more neutral environment. This causes excess scaling due to premature loss of corneocytes, much like what occurs in Netherton syndrome.
Putting It All Together
The invisible process of normal desquamation operates like a tightly choreographed ballet. The interplay between the proteases and their preferred protein diet (or ‘substrate’), as well as their activators and inhibitors, must all act together for the performance to come off. Isn’t it remarkable then, how often skin successfully accomplishes this task – so seamlessly and invisibly?
More than 40 different genes have been identified that when mutated cause some form of ichthyosis-like condition. Many of the genes that cause ichthyosis are only active in the skin – they don’t affect the function of other parts of the body. Thus, people affected by one of these genetic types may have skin issues (and complications from their abnormal skin), but do not have to be concerned about effects of these genes unrelated to skin function.
But some other forms of ichthyosis are caused by mutations of genes that are also active in other organs. These are multi-system genetic disorders, or ‘syndromic’ ichthyosis. The term ‘syndrome’ denotes a set of abnormalities affecting two or more organ systems.
All of these disorders have the ability to teach us much about how the skin (and, in the case of the syndromic forms, other parts of the body) operate(s). As we learn more about each of these forms and their underlying genetic causes, we not only expand our understanding of the human body but also we raise the possibility of developing new and more effective treatments.
Take as an example, a rare entity called CHILD syndrome. The discovery that the missing enzyme in this condition was required for the skin to produce the cholesterol it needs for its permeability barrier, has led to a successful topical treatment that both replaces the missing cholesterol and prevents formation of pathogenic intermediates. This type of ‘pathogenesis based therapy’ holds promise for the future treatments of other types of ichthyosis, as their underlying causes and mechanisms of disease become better understood.
Leave a Reply